
You may have already followed Tarini’s journey and read how she navigated her struggle with PCOS. Growing up, Tarini’s mother had educated her well, and Tarini felt confident and prepared for her first period. However, like many Indian mothers, hers had missed one crucial detail: the difference between “normal period pain” and signs of an underlying condition. She taught Tarini that severe period pain was simply a “part of being a woman”—a rite of passage to be endured in silence. This is where the misunderstanding began, and for years, her PCOS went undiagnosed.
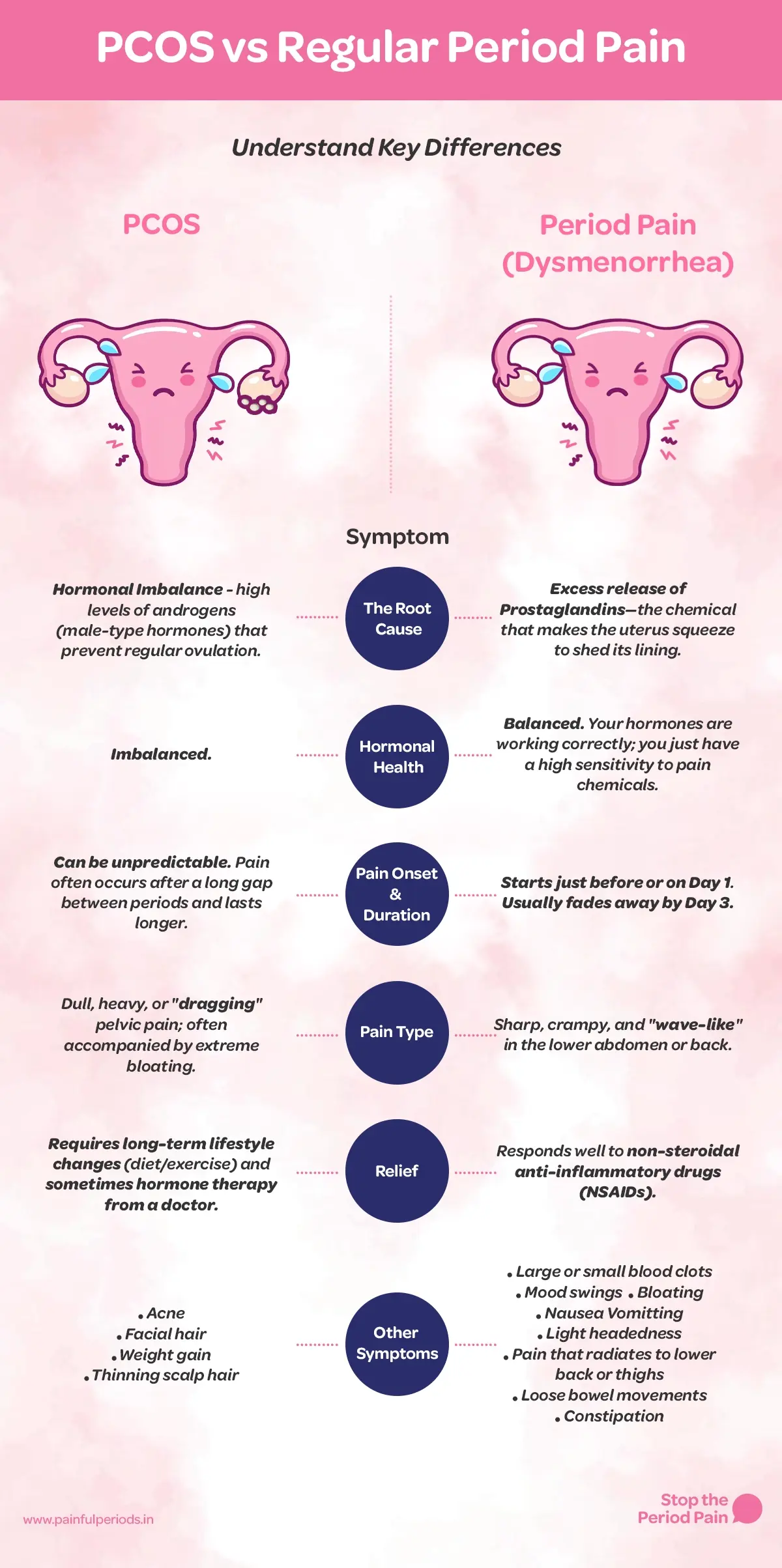
Let’s understand the differences between PCOS and regular period pain, so that you can be confident in knowing what is a normal part of your cycle and when it might be a sign of PCOS.
In This Story
What is regular period pain?
Regular period pain (medically known as dysmenorrhea) is the cramping sensation that accompanies your period. Almost all girls and women experience some degree of discomfort during their cycle.
The primary cause of this pain is the production of prostaglandins—natural chemicals in the body that signal the uterine muscles to contract. The rule is simple: More prostaglandins produced = More period pain.
While some discomfort is expected, period pain becomes a medical issue when:
- The pain is so severe that it results in significant discomfort.
- It impacts your daily life, forcing you to skip school, college, or work.
- It leaves you feeling exhausted or unable to concentrate.
The most important thing to remember about excessive period pain (dysmenorrhea) is this: apart from the excess production of prostaglandins, every other aspect of your menstrual health is correct. Your cycles are regular, your hormones are balanced, and your body is functioning as it should—it’s simply overproducing the “pain chemicals.”
Hit Up Our Period Pain Calculator
For real, how bad is your pain? Our interactive tool uses a 1-10 pain scale and a few quick questions to help you get the full picture. In just a few clicks, you’ll know if your pain is a chill or a major red flag.

What is PCOS?
PCOS (Polycystic Ovary Syndrome) is a hormonal condition that affects one in five Indian women. Unlike regular period pain, in which hormonal health is unaffected, PCOS involves a hormonal imbalance in the ovaries.
In a regular cycle, your ovaries release an egg every month (ovulation). In PCOS, the hormones that trigger this process get “confused.” This leads to two main issues:
- Irregular Cycles: Because the egg isn’t released on time, your periods may be late, unpredictable, or even stop for months.
- Thicker Lining, Heavier Pain: When your period finally arrives after a long gap, the lining of the uterus has become very thick. This causes the body to work extra hard to shed it, leading to much heavier bleeding and intense pain that can feel different from “regular” cramps.
PCOS involves more than just period pain
Because PCOS is a hormonal imbalance (specifically an increase in “androgens” or male-type hormones), it affects more than just your period. You might notice:
- Skin & Hair Changes: Persistent acne, thinning hair on the scalp, or unwanted hair growth on the face and body.
- Weight Fluctuations: Finding it very difficult to manage weight, especially around the midsection.
- Physical Signs: Darkened skin patches (often around the neck) or a general feeling of low energy.
Gynaecologist’s Advise:
When patients come to me with pain, the first thing I tell them is: “Pain is a signal, not a sentence.” Understanding your body is the key to treating it correctly.
- Listen to the Pattern: If your pain follows a predictable rhythm and your cycle is regular, you are likely dealing with a prostaglandin spike. In these cases, don’t wait for the pain to become unbearable. Using a targeted non-steroidal anti-inflammatory drug (NSAID) at the first sign of discomfort can block those “pain chemicals” before they take over your day.
- Look Beyond the Cramps: If you notice that your pain is accompanied by irregular periods, sudden acne, or unusual hair thinning, your body is signaling a hormonal shift like PCOS.
The Moral of the Story
The real tragedy of Tarini’s story wasn’t just the PCOS; it was the years she spent in silence, believing that her suffering was a mandatory part of being a woman. Her mother’s advice came from a place of love, but it was based on an old myth that “pain is normal.”
The lesson is simple: Being prepared for your period is good, but being empowered with the right facts is better.
While regular period pain (Dysmenorrhea) can be treated and stopped in its tracks, PCOS is a condition you learn to manage. It’s not about a “permanent cure,” but about lifestyle changes and the right medical support to keep your hormones in balance so they don’t control your life.
Be like the “new” Tarini: informed, confident, and proactive. Because once you understand your pain, you’ve already won half the battle.
More Stories To Read
Transform your understanding of period pain through engaging and informative stories based on real medical insights.
The Answers You've Been Looking For
Get clear, concise answers to your most pressing questions about period pain.
- Can Menstrual Pain Cause Depression?
- What is the cause of period pain?
- What are the symptoms of period pain?
- Why is my period so clotty and painful?
- What do large blood clots during period mean?
- When to see a doctor for painful periods?
- What will a gynaecologist do for painful periods?
- Can dysmenorrhea cause depression?
- What is the best treatment for period pain?
- How do you relieve period pain in teens?
Disclaimer:
This content is for informational purposes only and is not a substitute for professional medical advice. The information provided here is based on general trends and may not apply to every individual, as every woman’s body and experience with period pain is unique.
Do not self-diagnose or self-treat. If you are experiencing painful periods, especially if the pain is moderate to severe or accompanied by other concerning symptoms, you must consult with a gynaecologist. Ignoring severe period pain can lead to a significant delay in diagnosing underlying conditions that require proper medical attention. Always prioritise a confident conversation with your gynaecologist over self-treatment.






